Expanding Access to Health Care for Social Security Disability Insurance Beneficiaries: Early Findings from the Accelerated Benefits Demonstration
Social Security Bulletin, Vol. 70, No. 4, 2010
Most Social Security Disability Insurance (DI) beneficiaries must complete a 5-month waiting period before they become entitled to DI cash benefits and an additional 24-month waiting period before Medicare benefits begin. The Accelerated Benefits (AB) demonstration is a randomized experiment designed to test the effects of providing newly entitled DI beneficiaries who do not have health insurance with a generous health benefits package during the Medicare waiting period. This article presents early findings on the prevalence of health insurance coverage among newly entitled beneficiaries and the characteristics of those without health insurance. It also examines the effects of AB on health care utilization, the extent to which AB reduces unmet medical needs, and the costs of providing the AB health benefits package.
Robert Weathers is deputy associate commissioner, Office of Program Development and Research (OPDR), Social Security Administration (SSA). Chris Silanskis, Michelle Stegman, John Jones, and Susan Kalasunas are with the Office of Program Development, OPDR, SSA.
Acknowledgments: The authors are grateful to the following people for their comments on earlier versions of this article: Theresa Anderson, Susan Grad, Jeffrey Hemmeter, Nitin Jagdish, Bert Kestenbaum, Rene Parent, Incigul Sayman, Jim Sears, Sven Sinclair, and Michael Wiseman. The authors thank MDRC and Mathematica Policy Research, Inc. for providing us with the data we used for our analysis.
The findings and conclusions presented in the Bulletin are those of the authors and do not necessarily represent the views of the Social Security Administration.
Introduction
| AB | Accelerated Benefits |
| COBRA | Consolidated Omnibus Budget Reconciliation Act |
| DI | Disability Insurance |
| EBC | employment and benefits counseling |
| MCM | medical care management |
| MPR | Mathematica Policy Research, Inc. |
| PGAP | Progressive Goal Attainment Program |
| SSA | Social Security Administration |
Most Social Security Disability Insurance (DI) beneficiaries must complete a 5-month waiting period to qualify for cash benefits and an additional 24-month waiting period to qualify for Medicare. The 5-month waiting period begins with the first full calendar month after the onset of a disability.1 Some beneficiaries within either of the waiting periods may lose employer-provided health insurance coverage because their disability prevents them from working. Those who lose employer-provided health insurance may find it difficult to afford health insurance available through provisions of the Consolidated Omnibus Budget Reconciliation Act, commonly referred to as COBRA coverage.2 Other beneficiaries may not have had health insurance before disability onset and may find it difficult to obtain affordable health insurance coverage because of a preexisting condition. As a result, DI beneficiaries may not have access to the health care they need to address their disabling condition during the waiting period.
The popular press has used stories about a handful of beneficiaries to conclude that many beneficiaries within the 24-month Medicare waiting period do not have health insurance and that many may go without the health care needed to address their disabling condition. For example, one recent article uses the case of one beneficiary to infer a much larger problem, stating that many DI beneficiaries "have spent their savings on the care necessary to reach a diagnosis and now cannot get private insurance" (Saker 2010). Disability advocacy groups have stated that removing the Medicare waiting period may have the long-term benefit of increasing employment among beneficiaries. For example, the Consortium for Citizens with Disabilities has recommended eliminating the Medicare waiting period in order to help beneficiaries obtain the care required to stabilize their health condition and facilitate a transition to employment (CCD 2008). Yet policymakers lack the data to quantify the extent of the problem and the potential benefits of eliminating the Medicare waiting period.
Congress recognized the importance of health insurance coverage for individuals with disabilities in the "purpose and findings" section of the Ticket to Work and Work Incentives Improvement Act of 1999. Although the legislation did not alter the Medicare waiting period, it did authorize the Social Security Administration (SSA) to conduct a demonstration project designed to produce credible data on the costs and benefits of altering the 24-month Medicare waiting period. In 2005, SSA awarded a contract to MDRC, a nonprofit social policy research organization, to conduct the demonstration project. The project is called the Accelerated Benefits (AB) demonstration because it provides beneficiaries with a health benefits package before the completion of the Medicare waiting period.
This article describes the AB demonstration and the early findings from the project. The first section describes the core AB plan and the additional services available to some project participants. The second section describes the process used to identify, recruit, and enroll beneficiaries for the project, and presents findings from the enrollment process. The third section describes findings from the 6-month follow-up survey on AB service use and unmet medical needs. The fourth section presents data on AB health benefit expenditures and the characteristics of beneficiaries who reached the $100,000 health benefit limit. A discussion of the findings to date and future research plans concludes the article.
Project Design
The AB demonstration project was designed to determine whether providing a health benefits package and additional services during the 24-month Medicare waiting period would improve the health status of DI beneficiaries, increase the chances that they return to work, and reduce their reliance on DI cash benefits. We designed the project in collaboration with MDRC and their subcontractors.3 Key design features are described below.
Study Population and Study Sample
The study population for the AB demonstration project was DI beneficiaries who (1) were aged 18 to 54, (2) did not have health insurance coverage, (3) did not have a representative payee, and (4) were within the first 6 months of DI entitlement. Several studies indicated that this population group was likely to benefit from the AB plan and services. We selected a younger group because research has shown that younger recipients are more likely to return to work.4 We selected those without health insurance coverage because research has shown that they are more likely to have unmet medical needs, and thus could benefit from the AB plan.5 Excluding DI beneficiaries with health insurance also excluded beneficiaries who concurrently receive Supplemental Security Income (SSI) payments, because most SSI recipients receive Medicaid coverage. We selected those who did not have a representative payee because we wanted to obtain informed consent from the DI beneficiary. Finally, we selected those within the first 6 months of DI entitlement because we wanted to provide the AB package for a substantive period before the 24-month waiting period ended and Medicare began. Based on our assessment of prior research and on discussion with MDRC and MDRC's technical advisory group, we concluded that if the AB project does not have a substantive impact on our study population, then the AB program is unlikely to have a substantive impact for the broader population of DI beneficiaries.6
Our subcontractor, Mathematica Policy Research Inc. (MPR), selected a sample from the study population to test the impact of providing access to health benefits, either alone or in conjunction with additional services, to DI beneficiaries. MPR randomly assigned sample members into three groups: AB, AB Plus, and a control group. Participants in the AB and AB Plus groups had access to a health benefits package described below. In addition to health benefits, AB Plus members also received services designed to help them manage their health care, prepare for a return to work, and understand how employment might affect their benefits. We use the term "treatment group" to refer to the combined AB and AB Plus groups. The control group members did not receive access to health benefits, but they were not prohibited from obtaining health insurance through other means.
Health Benefits Package
The AB health plan covered a range of services designed to meet both general and specific health care needs of DI beneficiaries. The plan included basic hospital, medical, and drug benefits along with some nontraditional benefits including use of skilled nursing facilities, home health care, hospice care, prosthetics, dental care, nutritional counseling, and out-of-network services under certain circumstances.
No premiums were charged to individuals enrolled in the AB health plan. Participants were responsible for a $12 copayment for most services; exceptions were ambulatory and emergency room services ($35) and inpatient care ($200). Although the plan covered 100 percent of most services, participants were subject to a maximum health care benefit of $100,000. Limits were also placed on inpatient treatment for mental disorders, chemical abuse treatment, skilled nursing facility use, rehabilitation facility care, and home health care services. Certain procedures, services, and supplies required precertification or a utilization review to ensure that they were medically necessary.7
In addition to standard medical services, the AB health plan offered coverage for vision, hearing, and dental services. For vision care, the plan covered up to $200 for refraction, lenses, frames, and contact lenses. Hearing test and hearing aid costs were fully covered up to a $1,000 maximum benefit. The AB dental plan covered 100 percent of preventive/diagnostic (routine) services, 75 percent of basic services, and 50 percent of major services. Dental coverage was limited to a maximum benefit of $1,000.
The plan covered most prescription drugs after copayments of $5 for generic drugs, $15 for preferred brand name drugs, and $30 for nonpreferred brand name drugs.
AB Plus Services
AB Plus members received additional services that were not available to the AB and control group members. The first of these services was medical care management (MCM) provided by CareGuide, a health care management company. Each participant received a primary care manager, either a coach or a nurse, as determined by a preliminary assessment.8 Coaches provided beneficiaries with information on specific disorders, behavioral coaching, and assistance with obtaining health care. Nurses assessed clinical needs and assisted with navigating the health care system. These primary care managers monitored health care needs and adherence to treatment protocols, and helped coordinate health care for the participant.
Once participants achieved sufficient medical stabilization, they could begin the Progressive Goal Attainment Program (PGAP). PGAP is designed "to reduce psychosocial barriers to rehabilitation progress, promote re-integration into life-role activities, increase quality of life, and facilitate return-to-work" (University Centre 2010). MDRC recommended PGAP based on evidence that suggested it could be effective in improving functioning and could increase the likelihood of a return to work for individuals with a disability (Sullivan and others 2005). Because SSA disability determinations require DI claimants to be incapable of performing substantial gainful work, beneficiaries may have the false perception that they are unable to engage in activities that may lead to an eventual return to work. We thought PGAP could help beneficiaries overcome this perception. AB Plus participants were sent a PGAP video and workbook, and CareGuide coaches worked with AB Plus participants by telephone to help them complete PGAP.
AB Plus staff referred participants who showed interest in learning more about employment, and how it may affect their benefits, to employment and benefits counseling (EBC). EBC included discussion about the participant's work history, credentials, career goals, and employment expectations. Counselors also notified participants of local support services and helped prepare them for a return to work. Participants were given information on how employment could affect their benefits, reporting requirements, and work incentives. Transcen, Inc. provided EBC service by telephone.
Hypotheses
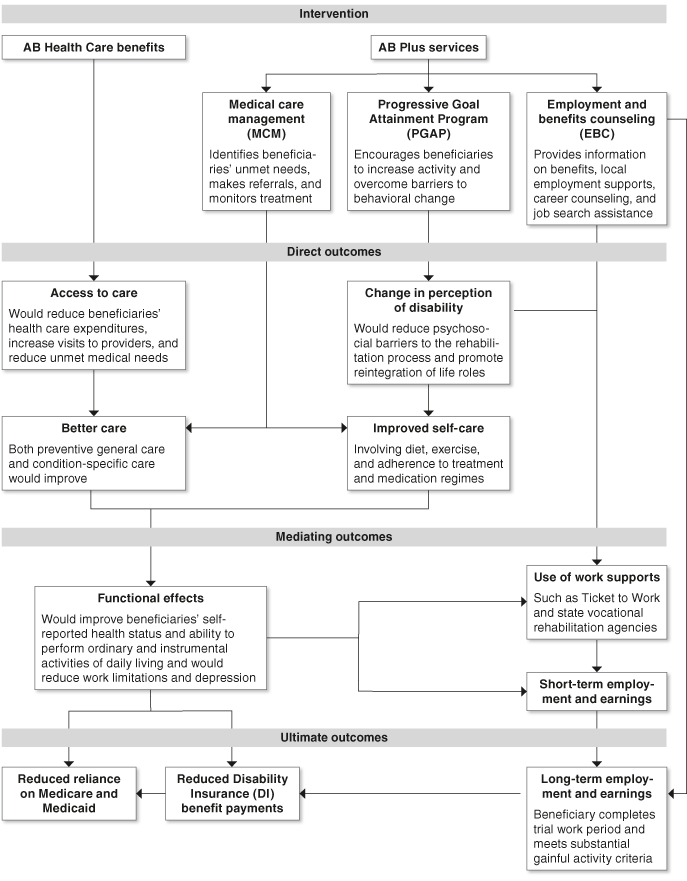
We hypothesize that the AB package will initially increase access to health care and reduce unmet health care needs among our study population (Chart 1). We also expect to see an increase in preventive care and quality of care overall. These direct outcomes should lead to improved functioning and health status, which may result in a return to work for some participants. The expected long-term outcomes include a reduction in DI benefits resulting from an increase in long-term employment and a reduction in future expenditures of public health insurance programs, such as Medicare and Medicaid, resulting from increased preventive care.
Anticipated flow of outcomes in Accelerated Benefits (AB) and AB Plus study groups
Text description for Chart 1.
Anticipated flow of outcomes in Accelerated Benefits (AB) and AB Plus study groups
Chart 1 is a flow chart with fifteen labeled boxes linked by arrows. There are four starting points in the flow chart. The flow is one-directional; that is, none of the arrows point back to a previous box, although some arrows laterally connect boxes that descend from different starting points. The flows are divided into four distinct panels labeled intervention, direct outcomes, mediating outcomes, and ultimate outcomes.
The starting points represent benefits or services provided to members of the two treatment groups in the Advanced Benefits (AB) demonstration project. The treatment groups are AB Health Care benefits and AB Plus services. The AB Health Care benefits package represents one starting point. The other three starting points comprise the three distinct services provided under AB Plus.
The flows originating with each starting point are presented as lists.
Starting point A
- Intervention: AB Health Care benefits.
- Direct outcome: Access to care. Would reduce beneficiaries' health care expenditures, increase visits to providers, and reduce unmet medical needs.
- Direct outcome: Better care. Both preventive general care and condition-specific care would improve.
- Direct outcome: Improved self-care involving diet, exercise, and adherence to treatment and medication regimes.
- Mediating outcome: Functional effects. Would improve beneficiaries' self-reported health status and ability to perform ordinary and instrumental activities of daily living and would reduce work limitations and depression.
- Mediating outcome: Use of work supports such as Ticket to Work and state vocational rehabilitation agencies.
- Mediating outcome: Short-term employment and earnings.
- Ultimate outcome: Long-term employment and earnings. Beneficiary completes trial work period and meets substantial gainful activity criteria.
- Ultimate outcome: Reduced Disability Insurance (DI) benefit payments.
- Ultimate outcome: Reduced reliance on Medicare and Medicaid.
Starting point B
- Intervention: AB Plus services, Medical care management (MCM). Identifies beneficiaries' unmet needs, makes referrals, and monitors treatment.
- Direct outcome: Better care. Both preventive general care and condition-specific care would improve.
- Direct outcome: Improved self-care involving diet, exercise, and adherence to treatment and medication regimes.
- Mediating outcome: Functional effects. Would improve beneficiaries' self-reported health status and ability to perform ordinary and instrumental activities of daily living and would reduce work limitations and depression.
- Mediating outcome: Use of work supports such as Ticket to Work and state vocational rehabilitation agencies.
- Mediating outcome: Short-term employment and earnings.
- Ultimate outcome: Long-term employment and earnings. Beneficiary completes trial work period and meets substantial gainful activity criteria.
- Ultimate outcome: Reduced Disability Insurance (DI) benefit payments.
- Ultimate outcome: Reduced reliance on Medicare and Medicaid.
Starting point C
- Intervention: AB Plus services, Progressive Goal Attainment Program (PGAP). Encourages beneficiaries to increase activity and overcome barriers to behavioral change.
- Direct outcome: Change in perception of disability. Would reduce psychosocial barriers to the rehabilitation process and promote reintegration of life roles.
- Direct outcome: Improved self-care—involving diet, exercise, and adherence to treatment and medication regimes.
- Direct outcome: Better care. Both preventive general care and condition-specific care would improve.
- Mediating outcome: Functional effects. Would improve beneficiaries' self-reported health status and ability to perform ordinary and instrumental activities of daily living and would reduce work limitations and depression.
- Mediating outcome: Use of work supports—such as Ticket to Work and state vocational rehabilitation agencies.
- Mediating outcome: Short-term employment and earnings.
- Ultimate outcome: Long-term employment and earnings. Beneficiary completes trial work period and meets substantial gainful activity criteria.
- Ultimate outcome: Reduced Disability Insurance (DI) benefit payments.
- Ultimate outcome: Reduced reliance on Medicare and Medicaid.
Starting point D
- Intervention: AB Plus services, employment and benefits counseling (EBC). Provides information on benefits, local employment supports, career counseling, and job search assistance.
- Mediating outcome: Use of work supports—such as Ticket to Work and state vocational rehabilitation agencies.
- Mediating outcome: Short-term employment and earnings.
- Ultimate outcome: Long-term employment and earnings. Beneficiary completes trial work period and meets substantial gainful activity criteria.
- Ultimate outcome: Reduced Disability Insurance (DI) benefit payments.
- Ultimate outcome: Reduced reliance on Medicare and Medicaid.
The AB Plus services provide additional supports to participants through three components as shown in Chart 1. MCM service helps participants adhere to the proper course of treatment. This can reduce the incidence of secondary health conditions that arise from deviations from a medical treatment regime, lead to additional improvements in overall health and functioning, increase chances of employment, and reduce reliance on public benefits. We hypothesize that PGAP will help beneficiaries change their attitudes toward their disabling condition and increase their motivation. Participants with higher motivation and a positive attitude may be more likely to seek work support programs and employment. EBC services will provide additional employment-related services, which should lead to higher reemployment and reduced reliance on public benefits.
AB Demonstration Not Designed to Estimate Induced Entry
The AB demonstration project will not produce an estimate of induced entry into the DI program. Induced entry may occur when DI changes involve new benefits or services that induce some individuals with disabilities to enter the program. Induced entry effects are difficult to estimate and, for DI, small increases in induced entry can translate into substantial program costs. Because the costs would increase significantly if we designed the demonstration to estimate induced entry effects and the complexity of such a design would have introduced substantial risks, we decided against developing a project with that capability.9
Recruitment Process
The AB demonstration recruitment goal was to enroll 2,000 uninsured DI beneficiaries. Our original intent was to assign 20 percent to the AB group, 40 percent to the AB Plus group, and 40 percent to the control group. As discussed later, however, health care costs necessitated a revised allocation. Ultimately, AB enrolled 2,005 participants: 616 (31 percent) in the AB Plus group, 401 (20 percent) in the AB group, and 988 (49 percent) in the control group. One AB Plus participant dropped out of the study, bringing the final total to 615.
We used SSA administrative records to identify newly entitled beneficiaries aged 18–54 who had to wait at least 18 months for Medicare entitlement and who were their own payees. Restricting the pool to beneficiaries who had at least 18 months left in the waiting period excluded a large number of beneficiaries who received an award notification letter after this period. Thus, we excluded beneficiaries who received benefits based on an appeal of their initial disability determination. We sent a monthly administrative data file to MPR, the subcontractor responsible for recruiting. Each file contained a new set of beneficiaries meeting our selection criteria. MPR sent a letter with information about the demonstration to a sample of beneficiaries identified in the file. A few days after sending the letter, MPR phoned those who agreed to participate to determine whether they had health insurance and were cognitively able to provide informed consent. Respondents who reported that they did not have health insurance at the time of the interview, and who could provide informed consent, completed a baseline survey that elicited information about their overall health status, use of medical services, employment history, attitudes toward work, household and demographic characteristics, and income; and whether they sought employment support services.10 Immediately upon finishing the survey, the MPR interviewer used a computerized random assignment algorithm to identify whether the participant was assigned to the AB Plus group, the AB group, or the control group. The MPR interviewer informed participants randomized into the AB or AB Plus groups of their assignment during their phone interview. MPR informed participants assigned to the control group by mail.
We used a two-phase recruitment strategy. The first phase was a demonstration pilot to guide the implementation of the larger second phase. The enrollment rates for both phases were exceptionally high, with 100 percent of the eligible Phase 1 beneficiaries and 99 percent of the eligible Phase 2 beneficiaries agreeing to participate.
Phase 1 began in October 2007 in four metropolitan areas—Houston, Minneapolis, New York City, and Phoenix. We sent MPR two administrative data files, one drawn at the end of September 2007 and one drawn at the end of October 2007. MPR sent letters to 1,503 beneficiaries in the 4 sites and 358 of the beneficiaries completed the health insurance questionnaire. Of those who completed the questionnaire, 70 candidates (19.6 percent) did not have health insurance. MPR limited Phase 1 enrollment to 66 beneficiaries and did not contact 4 of the candidates. All of the remaining 66 beneficiaries agreed to participate and completed the baseline survey. Phase 1 enrollment ended in November 2007.
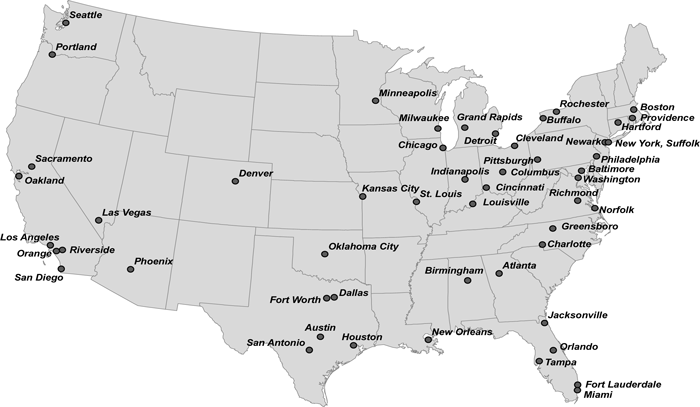
The first phase provided lessons to help recruitment in the second phase of the demonstration. Given the larger enrollment target of 1,934 participants in Phase 2, site selection required particular consideration of managing project costs.11 We determined that major metropolitan areas with high concentrations of DI beneficiaries would be the best locations and selected the largest 53 metropolitan areas.12 Chart 2 is a map showing the Phase 2 sites. We discontinued enrollment in (and dropped from the demonstration) Buffalo, because high rates of insured beneficiaries resulted in low enrollment; and Boston, because a change in state law mandated universal health insurance.
Accelerated Benefits study Phase 2 sites
Text description for Chart 2.
Accelerated Benefits study Phase 2 sites
Atlanta, Georgia
Austin, Texas
Baltimore, Maryland
Birmingham, Alabama
Boston, Massachusetts-New Hampshire
Buffalo, New York
Charlotte, North Carolina-South Carolina
Chicago, Illinois
Cincinnati, Ohio-Kentucky-Indiana
Cleveland, Ohio
Columbus, Ohio
Dallas, Texas
Denver, Colorado
Detroit, Michigan
Fort Lauderdale, Florida
Fort Worth, Texas
Grand Rapids, Michigan
Greensboro, North Carolina
Hartford, Connecticut
Houston, Texas
Indianapolis, Indiana
Jacksonville, Florida
Kansas City, Missouri-Kansas
Las Vegas, Nevada-Arizona
Los Angeles, California
Louisville, Kentucky-Indiana
Miami, Florida
Milwaukee, Wisconsin
Minneapolis, Minnesota-Wisconsin
Nassau-Suffolk, New York
Newark, New Jersey
New Orleans, Louisiana
New York, New York
Norfolk, Virginia-North Carolina
Oakland, California
Oklahoma City, Oklahoma
Orlando, Florida
Orange County, California
Philadelphia, Pennsylvania-New Jersey
Phoenix, Arizona
Pittsburgh, Pennsylvania
Portland, Oregon-Washington
Providence, Rhode Island-Massachusetts
Richmond, Virginia
Riverside, California
Rochester, New York
Sacramento, California
San Antonio, Texas
San Diego, California
Seattle, Washington
St. Louis, Missouri-Illinois
Tampa, Florida
Washington DC area
Phase 2 recruitment began in March 2008. We used the same recruitment procedures as in Phase 1, with only minor changes to the baseline survey. We sent monthly administrative record files to MPR beginning in February 2008 and continuing through December 2009. MPR sampled 21,109 of the 25,953 beneficiaries identified by SSA administrative files as meeting the demonstration's eligibility criteria. MPR contacted 17,876 beneficiaries by telephone and of those, 15,796 completed the health insurance question. The screening determined that 1,979 beneficiaries did not have health insurance and were eligible to participate, and MPR randomized 1,939 beneficiaries into the three study groups.
In November 2008, we stopped enrolling beneficiaries in the AB Plus study group. The original enrollment target for AB Plus was 800 participants, but we capped enrollment at 616 to contain costs. Health benefit expenditures for the Phase 1 sample were 50 percent higher than expected, and our estimates indicated that the budget could not support enrollment of 800 AB Plus participants. We determined that we would need to observe larger program benefits to justify the higher health benefit costs, and the final AB Plus sample size was statistically sufficient to identify important effects. To partially compensate for the loss in statistical precision associated with the smaller sample size, we expanded the control group from 800 to 1,000.
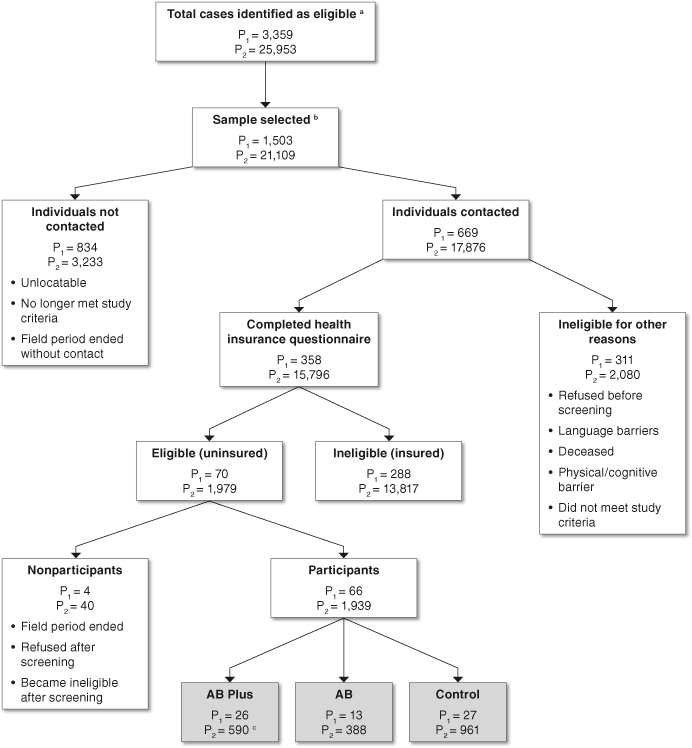
When Phase 2 enrollment ended in January 2009, 1,939 beneficiaries were enrolled, with 590 participants in the AB Plus group, 388 in the AB group, and 961 in the control group. One member of the AB Plus group dropped out of the study, lowering the Phase 2 enrollment to 589 participants. Chart 3 summarizes the case flow for both phases of the project.
Accelerated Benefits (AB) study population selection
Text description for Chart 3.
Accelerated Benefits (AB) study population selection
Chart 3 is a flow chart with thirteen labeled boxes linked by arrows. The flow is one-directional; that is, none of the arrows point back to a previous box.
The chart presents the seven-level process of selecting the population that ultimately participated in the Advanced Benefits (AB) demonstration project. Each box represents a population subgroup and includes a title identifying that subgroup and the number of people in Phase 1 and Phase 2 of the project comprising that subgroup. Boxes for subgroups that were excluded from the project sometimes also include reasons for exclusion. Some boxes include explanatory notes.
The boxes are arranged by level and described individually below. Those that flow to the next level are noted.
1. Title: Total cases identified as eligible. Numbers: Phase 1, 3,359; Phase 2, 25,953. Note: Social Security Administration (SSA) identified beneficiaries as meeting initial eligibility criteria based on administrative data and provided a list of these beneficiaries to Mathematica Policy Research, Inc. (MPR). Box 2 descends from this box.
2. Title: Sample selected. Numbers: Phase 1, 1,503; Phase 2, 21,109. Note: MPR selected a random sample of the beneficiaries identified by SSA and sent them a letter describing the demonstration project and inviting them to participate. Boxes 3A and 3B descend from this box.
3A. Title: Individuals not contacted: Numbers: Phase 1, 834; Phase 2, 3,233. Reasons not contacted: unlocatable, no longer met study criteria, or field period ended without contact.
3B. Title: Individuals contacted. Numbers: Phase 1, 669; Phase 2, 17,876. Boxes 4A and 4B descend from this box.
4A. Title: Completed health insurance questionnaire. Numbers: Phase 1, 358; Phase 2, 15,796. Boxes 5A and 5B descend from this box.
4B. Title: Ineligible for other reasons. Numbers: Phase 1, 311; Phase 2, 2,080. Reasons ineligible: refused before screening, language barriers, deceased, physical or cognitive barrier, or did not meet study criteria.
5A. Title: Eligible (uninsured). Numbers: Phase 1, 70; Phase 2, 1,979. Boxes 6A and 6B descend from this box.
5B. Title: Ineligible (insured). Numbers: Phase 1, 288; Phase 2, 13,817.
6A. Title: Nonparticipants. Numbers: Phase 1, 4; Phase 2, 40. Reasons not participating: field period ended, refused after screening, or became ineligible after screening.
6B. Title: Participants. Numbers: Phase 1, 66; Phase 2, 1,939. Boxes 7A, 7B, and 7C descend from this box.
7A. Title: AB Plus group. Numbers: Phase 1, 26; Phase 2, 590. Note: One AB Plus participant dropped out of the study after randomization.
7B. Title: AB group. Numbers: Phase 1, 13; Phase 2, 388.
7C. Title: Control group. Numbers: Phase 1, 27; Phase 2, 961.
Prevalence and Type of Health Insurance Coverage
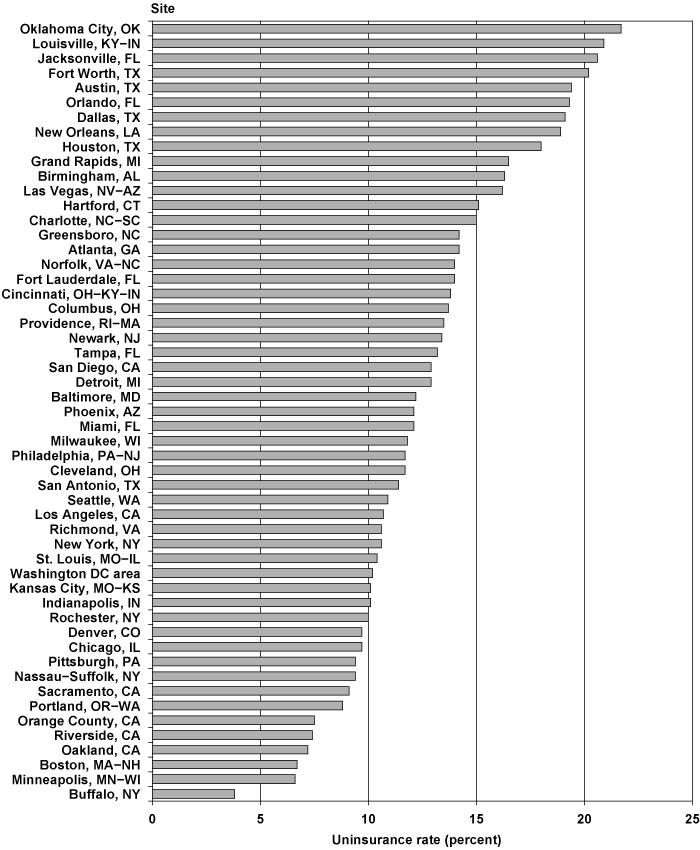
Given that 16,154 screened beneficiaries (358 in Phase 1 plus 15,796 in Phase 2) responded to all of the health insurance questions, and 2,049 (70 in Phase 1 plus 1,979 in Phase 2) were without insurance, the overall rate of those without health insurance was 12.7 percent. This rate varied substantially across the 53 sites, as shown in Chart 4. The highest rates of beneficiaries without health insurance were in Oklahoma City, Louisville, two sites in Florida, New Orleans, and four sites in Texas. The lowest rates were in Buffalo, Minneapolis, Boston, and several sites in California.
Uninsurance rate among Disability Insurance (DI) beneficiaries selected and contacted for Accelerated Benefits (AB) study, by site
| Metropolitan Area | Uninsurance Rate |
|---|---|
| Oklahoma City, Oklahoma | 21.7 |
| Louisville, Kentucky-Indiana | 20.9 |
| Jacksonville, Florida | 20.6 |
| Fort Worth, Texas | 20.2 |
| Austin, Texas | 19.4 |
| Orlando, Florida | 19.3 |
| Dallas, Texas | 19.1 |
| New Orleans, Louisiana | 18.9 |
| Houston, Texas | 18.0 |
| Grand Rapids, Michigan | 16.5 |
| Birmingham, Alabama | 16.3 |
| Las Vegas, Nevada-Arizona | 16.2 |
| Hartford, Connecticut | 15.1 |
| Charlotte, North Carolina-South Carolina | 15.0 |
| Greensboro, North Carolina | 14.2 |
| Atlanta, Georgia | 14.2 |
| Norfolk, Virginia-North Carolina | 14.0 |
| Fort Lauderdale, Florida | 14.0 |
| Cincinnati, Ohio-Kentucky-Indiana | 13.8 |
| Columbus, Ohio | 13.7 |
| Providence, Rhode Island-Massachusetts | 13.5 |
| Newark, New Jersey | 13.4 |
| Tampa, Florida | 13.2 |
| San Diego, California | 12.9 |
| Detroit, Michigan | 12.9 |
| Baltimore, Maryland | 12.2 |
| Phoenix, Arizona | 12.1 |
| Miami, Florida | 12.1 |
| Milwaukee, Wisconsin | 11.8 |
| Philadelphia, Pennsylvania-New Jersey | 11.7 |
| Cleveland, Ohio | 11.7 |
| San Antonio, Texas | 11.4 |
| Seattle, Washington | 10.9 |
| Los Angeles, California | 10.7 |
| Richmond, Virginia | 10.6 |
| New York, New York | 10.6 |
| St. Louis, Missouri-Louisiana | 10.4 |
| Washington DC area | 10.2 |
| Kansas City, Missouri-Kansas | 10.1 |
| Indianapolis, Indiana | 10.1 |
| Rochester, New York | 10.0 |
| Denver, Colorado | 9.7 |
| Chicago, Illinois | 9.7 |
| Pittsburgh, Pennsylvania | 9.4 |
| Nassau-Suffolk, New York | 9.4 |
| Sacramento, California | 9.1 |
| Portland, Oregon-Washington | 8.8 |
| Orange County, California | 7.5 |
| Riverside, California | 7.4 |
| Oakland, California | 7.2 |
| Boston, Massachusetts-New Hampshire | 6.7 |
| Minneapolis, Minnesota-Wisconsin | 6.6 |
| Buffalo, New York | 3.8 |
The baseline survey that identified whether a beneficiary had health insurance also provided data on the source of coverage for the insured. Among the 14,105 beneficiaries who reported health insurance coverage, 27.8 percent had insurance through an employer, 29.5 percent were covered by a spouse's plan, and 15.6 percent were covered through COBRA (Table 1). Nearly 32 percent of insured beneficiaries had coverage from public sources, with almost 18 percent insured through Medicaid or Medicare.13 About 8 percent had coverage through both a private and public plan.
| Type of insurance | Phase 1 | Phase 2 | Total |
|---|---|---|---|
| Any public | 26.3 | 31.7 | 31.6 |
| Medicare/Medicaid | 15.2 | 17.6 | 17.6 |
| Military health care benefits | 5.2 | 7.9 | 7.8 |
| Indian Health Service | 0.0 | 0.3 | 0.3 |
| Workers' compensation | 5.2 | 4.0 | 4.0 |
| Other state plan | 4.8 | 4.6 | 4.6 |
| Any private | 74.7 | 75.8 | 75.8 |
| Beneficiary's current/former employer | 26.3 | 27.8 | 27.8 |
| Spouse's current/former employer | 27.7 | 29.5 | 29.5 |
| Self- or family-paid | 5.2 | 5.0 | 5.0 |
| COBRA | 20.4 | 15.5 | 15.6 |
| Other | 0.0 | 1.8 | 1.8 |
| Sample size | 288 | 13,817 | 14,105 |
| SOURCE: Mathematica Policy Research, Inc., Accelerated Benefits (AB) demonstration project baseline survey, October 2007–January 2009. | |||
| NOTES: COBRA = Consolidated Omnibus Budget Reconciliation Act. | |||
| The sums of the values by coverage type may exceed the "any public" and "any private" subtotals because beneficiaries may have more than one type of coverage. Likewise, the sum of the "any public" and "any private" subtotals may exceed 100 because beneficiaries may have both. | |||
Characteristics of Those with Health Insurance Compared with Those without Coverage
Table 2 compares the age, sex, and impairment characteristics of three groups of beneficiaries identified for the study—the entire set of beneficiaries who were sent a letter about the AB project, the subset who reported having health insurance coverage, and the subset who agreed to participate in the study. Participants are similar to the group with health insurance in terms of age at entitlement and distribution by sex: Nearly 30 percent of each group are younger than 45, about 70 percent are aged 45–55, and a little over 49 percent are women. These groups are slightly older and have a larger percentage of female beneficiaries than the entire selected sample, where 69 percent were in the older age category and about 48 percent were women. There are differences in the distributions of impairment types between the groups. Participants are more likely than those reporting health insurance coverage to have mental disorders (22.0 percent versus 15.0 percent), diseases of the circulatory system (11.7 percent versus 8.7 percent), diseases of the musculoskeletal system and connective tissue (19.4 percent versus 14.0 percent), and diseases of the nervous system and sensory disorders (16.8 percent versus 14.8 percent). Participants are less likely to have neoplasms (8.2 percent) than beneficiaries who report that they have health insurance (23.8 percent).14
| Characteristic | Selected sample | Insured | Participants |
|---|---|---|---|
| Age | |||
| 44 or younger | 31.0 | 29.5 | 29.9 |
| 45 or older | 69.0 | 70.5 | 70.1 |
| Sex | |||
| Men | 52.2 | 50.9 | 50.2 |
| Women | 47.8 | 49.1 | 49.8 |
| Impairments | |||
| Mental disorders a | 15.8 | 15.0 | 22.0 |
| Neoplasms | 24.3 | 23.8 | 8.2 |
| Diseases of the— | |||
| Circulatory system | 9.1 | 8.7 | 11.7 |
| Musculoskeletal system and connective tissue | 13.4 | 14.0 | 19.4 |
| Nervous system and sense organs | 14.3 | 14.8 | 16.8 |
| Other b | 23.2 | 23.6 | 22.1 |
| Sample size | 22,612 | 14,105 | 2,005 |
| SOURCE: Authors' calculations based on Social Security administrative data. | |||
| a. Excludes mental retardation, which is categorized at "Other." | |||
| b. Includes congenital anomalies; endocrine, nutritional, and metabolic diseases; injuries; mental retardation; diseases of the blood and blood-forming organs, digestive system, genitourinary system, respiratory system, and skin and subcutaneous tissue; human immunodeficiency virus/acquired immune deficiency syndrome (HIV/AIDS); and other diagnoses. | |||
Characteristics of Project Participants from Baseline Survey
The baseline survey that MPR administered prior to randomization provided a more detailed description of beneficiaries who agreed to participate in the study. Table 3 presents the participants' demographic characteristics and includes information on their income, education, and homeownership status. Table 4 presents self-reported health, functional, and physical limitations in addition to primary diagnosis categories. Table 5 presents the health insurance coverage that participants reported having prior to randomization. Table 6 presents the percentage of reported unmet needs prior to randomization, with medical and prescription drug needs shown separately. All tables include p-values to help identify differences in characteristics across groups that arose by chance and that might be correlated with the AB outcomes specified in Chart 1. MDRC provided evidence that they implemented the assignment process properly and that any differences are due to chance and not to deviations from random assignment.
Most of our study sample had an annual household income below $30,000 (Table 3). Approximately 60 percent of the participants reported less than $30,000 in income; 16.6 percent reported having less than $10,000. Only 14.6 percent reported household income greater than $50,000. The large share of beneficiaries with annual household income of less than $30,000 indicates that many beneficiaries who enter the DI program without health insurance coverage may benefit from the recently passed health care reform, the Affordable Care Act. The law makes health insurance coverage more affordable by providing subsidies for families with income below 400 percent of the federal poverty line to purchase insurance through new health insurance exchanges.15 Many of the beneficiaries we contacted who did not have health insurance coverage were likely to meet the eligibility standards under the new law.
| Characteristic | AB Plus group | AB group | Control group | Total | P-value | Percentage missing a | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Annual household income (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.884 | 6.2 | ||||||||||||||||
| Less than $10,000 | 17.2 | 17.9 | 15.8 | 16.6 | . . . | . . . | ||||||||||||||||
| $10,000 to $19,999 | 21.0 | 19.2 | 21.8 | 21.0 | . . . | . . . | ||||||||||||||||
| $20,000 to $29,999 | 21.8 | 21.3 | 23.5 | 22.6 | . . . | . . . | ||||||||||||||||
| $30,000 to $39,999 | 15.3 | 17.1 | 14.6 | 15.3 | . . . | . . . | ||||||||||||||||
| $40,000 to $49,999 | 9.0 | 9.7 | 10.4 | 9.8 | . . . | . . . | ||||||||||||||||
| $50,000 or more | 15.8 | 14.7 | 13.9 | 14.6 | . . . | . . . | ||||||||||||||||
| Marital status (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.652 | 0.2 | ||||||||||||||||
| Married, living with spouse | 43.4 | 41.3 | 39.6 | 41.1 | . . . | . . . | ||||||||||||||||
| Unmarried, living with partner | 4.6 | 5.3 | 4.4 | 4.6 | . . . | . . . | ||||||||||||||||
| Married, not living with spouse | 6.5 | 5.3 | 7.0 | 6.5 | . . . | . . . | ||||||||||||||||
| Unmarried, not living with partner | 45.5 | 48.3 | 49.0 | 47.8 | . . . | . . . | ||||||||||||||||
| Families with any dependent children b (%) | 24.7 | 24.6 | 24.4 | 24.5 | 0.988 | 0.5 | ||||||||||||||||
| Educational attainment (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.399 | 0.1 | ||||||||||||||||
| General Educational Development (GED) | 7.3 | 7.0 | 6.7 | 6.9 | . . . | . . . | ||||||||||||||||
| High school diploma | 53.7 | 51.1 | 50.5 | 51.6 | . . . | . . . | ||||||||||||||||
| Technical certificate/associate's degree/2-year college program | 9.6 | 13.0 | 9.2 | 10.1 | . . . | . . . | ||||||||||||||||
| Four (or more) years of college | 8.1 | 8.2 | 9.8 | 9.0 | . . . | . . . | ||||||||||||||||
| None of the above | 21.3 | 20.7 | 23.8 | 22.4 | . . . | . . . | ||||||||||||||||
| Age group (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.103 | 0.0 | ||||||||||||||||
| 18–34 | 6.0 | 9.2 | 9.7 | 8.5 | . . . | . . . | ||||||||||||||||
| 35–44 | 21.8 | 22.7 | 20.6 | 21.4 | . . . | . . . | ||||||||||||||||
| 45–55 | 72.2 | 68.1 | 69.6 | 70.1 | . . . | . . . | ||||||||||||||||
| Average age (years) | 47.3 | 46.3 | 46.6 | 46.8* | 0.066 | 0.0 | ||||||||||||||||
| Sex (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.272 | 0.0 | ||||||||||||||||
| Men | 52.8 | 48.1 | 49.5 | 50.2 | . . . | . . . | ||||||||||||||||
| Women | 47.2 | 51.9 | 50.5 | 49.8 | . . . | . . . | ||||||||||||||||
| Race/ethnicity (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.585 | 0.7 | ||||||||||||||||
| White | 60.9 | 58.1 | 56.8 | 58.3 | . . . | . . . | ||||||||||||||||
| Black | 20.2 | 23.3 | 22.5 | 22.0 | . . . | . . . | ||||||||||||||||
| Hispanic | 14.4 | 13.0 | 14.7 | 14.3 | . . . | . . . | ||||||||||||||||
| Other | 4.4 | 5.5 | 6.0 | 5.4 | . . . | . . . | ||||||||||||||||
| Census region (%) | ||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.467 | 0.0 | ||||||||||||||||
| South | 46.8 | 42.9 | 46.6 | 45.9 | . . . | . . . | ||||||||||||||||
| Midwest | 17.7 | 21.7 | 19.0 | 19.2 | . . . | . . . | ||||||||||||||||
| West/Pacific | 18.5 | 17.0 | 19.1 | 18.5 | . . . | . . . | ||||||||||||||||
| Northeast | 16.9 | 18.5 | 15.3 | 16.4 | . . . | . . . | ||||||||||||||||
| Homeowner status (%) | 44.8 | 44.1 | 39.6 | 42.1 | 0.142 | 0.5 | ||||||||||||||||
| Sample size | 615 | 401 | 988 | 2,004 | ||||||||||||||||||
| SOURCES: MDRC calculations based on Social Security administrative data and Mathematica Policy Research, Inc., Accelerated Benefits (AB) demonstration project baseline survey, October 2007–January 2009. | ||||||||||||||||||||||
| NOTES: . . . = not applicable. | ||||||||||||||||||||||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance is indicated as * = 10 percent level. For categorical characterstics, the p-value and percentage missing apply to category totals only. | ||||||||||||||||||||||
| Additional tests were run to determine whether there was a difference in the distribution of the characteristics between specific pairs of study groups. | ||||||||||||||||||||||
The following tests were statistically significant:
|
||||||||||||||||||||||
| Totals do not necessarily equal the sum of rounded components. | ||||||||||||||||||||||
| a. Missing values are due to survey responses of "don't know" or refusals to answer the question. Respondents with missing values were excluded from calculations of percentage distributions, means, and tests of statistical significance of differences across study groups. | ||||||||||||||||||||||
| b. This measure includes children for whom the participant is a primary provider or caregiver. | ||||||||||||||||||||||
The data also provide a picture of the demographic characteristics of participants. The majority were between ages 45 and 55. The sample was nearly equally split between men and women. The majority of participants were white (58.3 percent), and 22.0 percent were black. A large portion of the demonstration's participants (45.9 percent) lived in the South, and 42.1 percent owned their own home. The majority (51.6 percent) of participants reported having a high school diploma, but nearly 20 percent had a higher education degree. There are no substantive differences in demographic or economic characteristics between the AB Plus group, the AB group, and the control group.
Not surprisingly, most beneficiaries reported substantial health impairments and functional limitations (Table 4). High percentages of participants reported having mental disorders (22.0 percent) or diseases of the musculoskeletal connective tissue and nervous system (19.4 percent). Table 4 also shows a difference between the three groups for the primary diagnosis of a neoplasm, which was reported by 10.6 percent of the AB Plus group, 8.2 percent of the AB group, and 6.7 percent of the control group. We are somewhat concerned about this difference because of the high incidence of death among beneficiaries with neoplasms during the 24-month waiting period, and accounting for this difference when analyzing mortality outcomes may be important. Over 94 percent of the randomized participants possess some form of disability that hinders their daily activities. Large shares of participants reported having difficulty standing for long periods (83.8 percent), climbing a flight of stairs (78.3 percent), or lifting or carrying a 10-pound package (62.7 percent). Participants also reported having difficulty preparing meals (36.6 percent), using public transportation (36.4 percent), taking medication (34.4 percent), and riding as a passenger in a car (21.1 percent). Over 80 percent reported some form of personal or emotional problems that hindered their daily activities in the 4 weeks preceding randomization. When the participants were asked the severity of their conditions, 34.9 percent reported they had "a lot" and 25.0 percent said they had "some" personal or emotional problems affecting their daily activities. A substantial share of participants (14.2 percent) reported they could not do daily activities.
| Characteristic | AB Plus group | AB group | Control group | Total | P-value | Percentage missing a | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Health and functional limitations (%) | ||||||||||||||||||||
| Primary diagnosis | ||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.349 | 0.0 | ||||||||||||||
| Mental disorders b | 20.2 | 22.7 | 22.9 | 22.0 | . . . | . . . | ||||||||||||||
| Neoplasms | 10.6 | 8.2 | 6.7 | 8.2 | . . . | . . . | ||||||||||||||
| Diseases of the— | ||||||||||||||||||||
| Circulatory system | 11.9 | 10.7 | 11.8 | 11.6 | . . . | . . . | ||||||||||||||
| Musculoskeletal system and connective tissue | 18.7 | 19.2 | 19.8 | 19.4 | . . . | . . . | ||||||||||||||
| Nervous system and sense organs | 15.4 | 16.5 | 17.7 | 16.8 | . . . | . . . | ||||||||||||||
| Other c | 23.3 | 22.7 | 21.1 | 22.1 | . . . | . . . | ||||||||||||||
| Difficulty with any instrumental activities of daily living (IADLs) | 94.1 | 93.5 | 94.3 | 94.1 | 0.842 | 0.0 | ||||||||||||||
| Standing for long periods | 85.3 | 83.0 | 83.3 | 83.8 | 0.501 | 0.2 | ||||||||||||||
| Climbing a flight of stairs | 79.8 | 77.9 | 77.5 | 78.3 | 0.550 | 0.3 | ||||||||||||||
| Lifting or carrying 10-pound package | 62.5 | 60.5 | 63.7 | 62.7 | 0.543 | 0.3 | ||||||||||||||
| Preparing meals | 31.5 | 36.9 | 39.6 | 36.6*** | 0.005 | 0.2 | ||||||||||||||
| Using public transportation | 35.1 | 34.1 | 38.2 | 36.4 | 0.265 | 2.6 | ||||||||||||||
| Taking medication | 34.6 | 36.2 | 33.5 | 34.4 | 0.632 | 0.1 | ||||||||||||||
| Riding as a passenger in a car | 20.2 | 20.5 | 21.9 | 21.1 | 0.664 | 0.2 | ||||||||||||||
| Using the telephone | 6.7 | 7.5 | 7.3 | 7.1 | 0.852 | 0.1 | ||||||||||||||
| Self-reported personal or emotional problems in last 4 weeks (%) | ||||||||||||||||||||
| Personal or emotional problems resulted in accomplishing less in daily activities | 82.0 | 78.7 | 81.6 | 81.1 | 0.376 | 0.9 | ||||||||||||||
| Personal or emotional problems affected daily activities— | ||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.688 | 0.2 | ||||||||||||||
| A lot | 37.0 | 34.3 | 33.9 | 34.9 | . . . | . . . | ||||||||||||||
| Some | 24.3 | 26.5 | 24.9 | 25.0 | . . . | . . . | ||||||||||||||
| A little | 16.0 | 15.3 | 15.7 | 15.7 | . . . | . . . | ||||||||||||||
| Not at all | 8.6 | 11.8 | 10.6 | 10.2 | . . . | . . . | ||||||||||||||
| Could not do daily activities | 14.2 | 12.3 | 14.9 | 14.2 | . . . | . . . | ||||||||||||||
| Sample size | 615 | 401 | 988 | 2,004 | ||||||||||||||||
| SOURCE: MDRC calculations based on Social Security administrative data and Mathematica Policy Research, Inc., AB demonstration project baseline survey, October 2007–January 2009. | ||||||||||||||||||||
| NOTES: . . . = not applicable. | ||||||||||||||||||||
| Totals do not necessarily equal the sum of rounded components. | ||||||||||||||||||||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance is indicated as *** = 1 percent level. For categorical characteristics, the p-value and percentage missing apply to category totals only. | ||||||||||||||||||||
| Additional tests were run to determine whether there was a difference in the distribution of the characteristics between specific pairs of study groups. | ||||||||||||||||||||
The following tests were statistically significant:
|
||||||||||||||||||||
| a. Missing values are due to survey responses of "don't know" or refusals to answer the question. Respondents with missing values were excluded from calculations of percentage distributions, means, and tests of statistical significance of differences across study groups. | ||||||||||||||||||||
| b. Excludes mental retardation, which is categorized as "Other." | ||||||||||||||||||||
| c. Includes congenital anomalies; endocrine, nutritional, and metabolic diseases; injuries; mental retardation; diseases of the blood and blood-forming organs, digestive system, genitourinary system, respiratory system, and skin and subcutaneous tissue; infectious and parasitic diseases; human immunodeficiency virus/acquired immune deficiency syndrome (HIV/AIDS); and other diagnoses. | ||||||||||||||||||||
Table 5 shows the health insurance history of participants. Less than 4 percent reported that they had never had health insurance prior to enrollment. Of the participants who reported having had health insurance, 85.3 percent reported having private insurance. Eight percent of participants who had health insurance coverage reported that they had public coverage either through Medicare or Medicaid.16 Over 62 percent of the participants reported having health insurance within the last year, with 36.1 percent reporting they had health insurance in the 6 months leading up to the baseline survey.
| Characteristic | AB Plus group | AB group | Control group | Total | P-value | Percentage missing a | ||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Type of last health insurance coverage (%) | ||||||||||||||||||||||||||||||
| Never insured | 3.8 | 4.0 | 3.9 | 3.9 | 0.984 | 1.1 | ||||||||||||||||||||||||
| Any private | 85.7 | 81.7 | 86.5 | 85.3* | 0.071 | 0.3 | ||||||||||||||||||||||||
| Beneficiary's current/former employer | 63.0 | 60.4 | 65.7 | 63.8 | 0.160 | 0.3 | ||||||||||||||||||||||||
| Spouse's current/former employer | 6.8 | 8.3 | 7.0 | 7.2 | 0.651 | 0.3 | ||||||||||||||||||||||||
| Self- or family-paid | 4.4 | 3.3 | 3.5 | 3.7 | 0.542 | 0.3 | ||||||||||||||||||||||||
| COBRA | 7.7 | 6.5 | 6.8 | 7.0 | 0.738 | 0.3 | ||||||||||||||||||||||||
| Other | 4.6 | 4.3 | 4.2 | 4.3 | 0.929 | 0.3 | ||||||||||||||||||||||||
| Any public | 11.7 | 15.8 | 10.5 | 11.9** | 0.021 | 0.3 | ||||||||||||||||||||||||
| Medicare or Medicaid | 7.0 | 9.8 | 7.8 | 8.0 | 0.274 | 0.3 | ||||||||||||||||||||||||
| Military health care benefits | 1.0 | 0.8 | 0.4 | 0.7 | b | 0.3 | ||||||||||||||||||||||||
| Indian Health Service | 0.0 | 0.0 | 0.1 | 0.1 | b | 0.3 | ||||||||||||||||||||||||
| Workers' compensation | 1.1 | 1.3 | 0.8 | 1.0 | 0.694 | 0.3 | ||||||||||||||||||||||||
| Other state plan | 2.6 | 4.0 | 1.3 | 2.3*** | 0.007 | 0.3 | ||||||||||||||||||||||||
| Date of last health insurance coverage (%) | ||||||||||||||||||||||||||||||
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 0.567 | 1.1 | ||||||||||||||||||||||||
| Less than 6 months ago | 36.8 | 40.2 | 34.0 | 36.1 | . . . | . . . | ||||||||||||||||||||||||
| 6 months to less than 1 year ago | 25.6 | 23.6 | 27.7 | 26.2 | . . . | . . . | ||||||||||||||||||||||||
| 1 year to less than 2 years ago | 13.0 | 14.3 | 14.0 | 13.8 | . . . | . . . | ||||||||||||||||||||||||
| 2 or more years ago | 20.8 | 17.8 | 20.4 | 20.0 | . . . | . . . | ||||||||||||||||||||||||
| Never insured | 3.8 | 4.0 | 3.9 | 3.9 | . . . | . . . | ||||||||||||||||||||||||
| Sample size | 615 | 401 | 988 | 2,004 | ||||||||||||||||||||||||||
| SOURCE: MDRC calculations based on Social Security administrative data and Mathematica Policy Research, Inc., AB demonstration project baseline survey, October 2007–January 2009. | ||||||||||||||||||||||||||||||
| NOTES: COBRA = Consolidated Omnibus Budget Reconciliation Act; . . . = not applicable. | ||||||||||||||||||||||||||||||
| Totals do not necessarily equal the sum of rounded components. The sums of the values by coverage type may exceed the "any public" and "any private" subtotals because beneficiaries may have had more than one type of coverage. Likewise, the sum of the "any public" subtotal, the "any private" subtotal, and "never insured" may exceed 100 because beneficiaries may have had both public and private coverage. | ||||||||||||||||||||||||||||||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance levels are indicated as * = 10 percent, ** = 5 percent, and *** = 1 percent. For categorical characteristics, the p-value and percentage missing apply to category totals only. | ||||||||||||||||||||||||||||||
| Additional tests were run to determine whether there was a difference in the distribution of the characteristics between specific pairs of study groups. | ||||||||||||||||||||||||||||||
The following tests were statistically significant:
|
||||||||||||||||||||||||||||||
| a. Missing values are due to survey responses of "don't know" or refusals to answer the question. Respondents with missing values were excluded from calculations of percentage distributions, means, and tests of statistical significance of differences across study groups. | ||||||||||||||||||||||||||||||
| b. Tests of statistical significance were not performed for differences among study groups because sample sizes were too small. | ||||||||||||||||||||||||||||||
A majority of participants reported unmet health care needs prior to randomization into the project. Table 6 shows that 70.2 percent of participants reported some form of unmet medical needs and 69.9 percent reported some type of unmet prescription need. It also shows that 57.7 percent reported having postponed getting medical care and 47.0 percent reported they did not get medical care they needed. When the category was combined, 64.7 percent reported they either did not get or postponed medical care they needed. Of the participants reporting unmet prescription needs, 53.9 percent reported that they used prescriptions less than prescribed, 53.7 percent reported they did not fill prescriptions when first prescribed, 51.5 percent reported they did not refill their prescriptions, and 47.8 percent did not fill entire prescriptions. There are no substantive differences in unmet medical needs between the three participant groups.
| Characteristic | AB Plus group | AB group | Control group | Total | P-value | Percentage missing a |
|---|---|---|---|---|---|---|
| Percentage of participants reporting— | ||||||
| Any unmet medical need | 71.1 | 69.8 | 69.8 | 70.2 | 0.859 | 0.0 |
| Postponed getting medical care | 58.1 | 57.9 | 57.4 | 57.7 | 0.959 | 0.2 |
| Did not get medical care | 47.5 | 47.6 | 46.5 | 47.0 | 0.907 | 0.5 |
| Referred to doctor, but did not go | 17.8 | 17.5 | 15.4 | 16.5 | 0.397 | 0.1 |
| Referred for surgery, but did not go | 16.8 | 18.3 | 15.6 | 16.5 | 0.459 | 0.3 |
| Referred for tests, but did not go | 10.5 | 8.8 | 8.6 | 9.2 | 0.441 | 0.3 |
| Did not get or postponed medical care | 64.4 | 64.8 | 64.9 | 64.7 | 0.979 | 0.0 |
| Any unmet prescription need | 69.3 | 69.3 | 70.4 | 69.9 | 0.853 | 0.0 |
| Used prescription less than prescribed | 55.6 | 52.6 | 53.4 | 53.9 | 0.580 | 0.0 |
| Did not fill prescription when first prescribed | 52.3 | 54.6 | 54.3 | 53.7 | 0.685 | 0.1 |
| Did not refill prescription | 51.9 | 52.3 | 51.0 | 51.5 | 0.897 | 0.0 |
| Did not fill entire prescription | 46.0 | 48.3 | 48.7 | 47.8 | 0.560 | 0.1 |
| Sample size | 615 | 401 | 988 | 2,004 | ||
| SOURCE: MDRC calculations based on Social Security administrative data and Mathematica Policy Research, Inc., AB demonstration project baseline survey, October 2007–January 2009. | ||||||
| a. Missing values are due to survey responses of "don't know" or refusals to answer the question. Respondents with missing values were excluded from calculations of percentage distributions, means, and tests of statistical significance of differences across study groups. | ||||||
Six-Month Follow-up Survey
MPR conducted a 6-month follow-up survey to gather timely information about the design and implementation of the intervention and to assess early impacts on health care utilization and unmet health care needs. To determine if the plan needed any modifications, we assessed participant satisfaction with plan design and implementation. The survey consisted of topic modules, with pertinent program topics comprising medical service use, unmet medical needs, health insurance coverage, and satisfaction with AB services. We planned to survey 600 participants (240 control, 120 AB, 240 AB Plus).17 MPR conducted the surveys using computer-assisted telephone interviewing (CATI). Survey operations began in October 2008 and were completed in January 2009. A total of 483 surveys (80.5 percent) were completed, covering 194 control group, 96 AB, and 193 AB Plus participants. MPR reported that nonrespondents included 5 refusals, 14 who were deceased, and 98 who were alive according to administrative records but could not be contacted.
Use of Benefits by Program Participants
Most of the participants who received the health benefits package through the project used at least one of the services that were available (86.5 percent of the AB Plus group and 87.3 percent of the AB group), as shown in Table 7. The survey also captured user satisfaction rates. We intended to use this information to make any necessary adjustments to the provision of services. However, satisfaction rates with the services provided were very high (mostly above 90 percent) with little variation between AB and AB Plus users.18 We view these results as indicating that our contractor and subcontractors delivered the AB and AB Plus services as we intended.
| Benefit or service | AB Plus | AB |
|---|---|---|
| Used any plan benefits (%) | 86.5 | 87.3 |
| Primary care | 70.2 | 67.4 |
| Specialty care | 55.1 | 52.8 |
| Mental health care | 13.5 | 18.7 |
| Dental care | 17.4 | 19.8 |
| Vision care | 19.0 | 18.6 |
| Prescription drug | 76.2 | 74.6 |
| Rehabilitation care | 12.5 | 13.3 |
| Medical equipment | 12.6 | 8.3 |
| Used any of the three additional services a (%) | 81.1 | . . . |
| CareGuide b | 78.1 | . . . |
| Employment and benefit counseling | 31.2 | . . . |
| Medical care management | 20.7 | . . . |
| Sample size | 193 | 96 |
| SOURCE: Mathematica Policy Research, Inc., AB demonstration project 6-month followup survey, October 2008–January 2009. | ||
| NOTES: . . . = not applicable. | ||
| Sample sizes vary according to benefit use. Estimates are weighted for nonresponse. | ||
| a. Respondents were considered to have "any use" of each of the three services if they reported they had "been in touch" with the staff. Use of the individual services was indicated if participants reported "interactions" with coaches, counselors, or nurses who provided those services. | ||
| b. May reflect the intake assessment, use of the Progressive Goal Attainment Program, and other contacts in which the coach helps coordinate participant's access to the other AB components. | ||
The most commonly used service for participants in both groups was the prescription drug benefit, followed by primary care and specialty care. It is somewhat surprising that the service-use rates of the program groups are very similar. During the design phase, our technical advisory group and contractor indicated that the MCM model would increase use of available health benefits. We thought this would be particularly true in our study because participants did not have health insurance and perhaps had limited recent experience in dealing with health care providers. The similarity in health benefits use among the groups may be due to a common unsatisfied demand for services resulting from the lack of health insurance. In addition, within 6 months of enrollment, only 20.7 percent of the participants had used the MCM services.
The high rate of use of the CareGuide coaches (78.1 percent) shown in Table 7 may reflect the fact that these coaches were part of the AB Plus intake process. The coaches did an initial assessment to determine whether the participant needed referral to the MCM nurses or was ready to begin the PGAP program.
Control Group Members Getting Health Insurance
At the time of random assignment, no participants had health insurance coverage. Table 8 shows the percentage of participants in the treatment group (that is, members of either the AB or AB Plus groups) and in the control group who reported that they were able to obtain some other type of health insurance during the first 6 months. We were somewhat surprised that 24.2 percent of the control group was able to obtain health insurance coverage within 6 months of random assignment; 10.7 percent of control group members, or nearly half (about 44 percent) of control group members who obtained health insurance, were covered through a public source. Apparently, we underestimated the likelihood that DI beneficiaries might become qualified for Medicaid through "spend down" provisions, or covered under other state programs. Table 8 also shows that 15.0 percent of all control group members reported obtaining some type of private health insurance coverage, accounting for about 62 percent of the control group who had health insurance coverage.19 Although we expected this to be difficult because of their health status, apparently we underestimated the likelihood that participants would purchase coverage from a former employer (through COBRA) or obtain it through a spousal plan. The small percentage (1.5) of treatment group members who picked up additional private insurance reflects the fact that these plans are costly and would likely duplicate the services provided by the AB package.
| Type of coverage | AB and AB Plus combined | Control group | P-value |
|---|---|---|---|
| Any nonproject insurance a | 15.8 | 24.2 | 0.020** |
| Private insurance b | 1.5 | 15.0 | <0.001*** |
| Public insurance c | 14.9 | 10.7 | 0.180 |
| No nonproject insurance | 84.2 | 75.8 | 0.020** |
| Sample size | 289 | 194 | |
| SOURCE: Mathematica Policy Research, Inc., AB demonstration project 6-month followup survey, October 2008–January 2009. | |||
| NOTES: Estimates are regression adjusted to account for chance baseline differences across the study groups and weighted for nonresponse. A small percentage of cases had missing values; these were interpreted as not having coverage. The p-value column represents the probability that the differences between the characteristics of the treatment and control groups are different from zero. | |||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance levels are indicated as ** = 5 percent and *** = 1 percent. | |||
| a. The sum of private and public insurance exceeds the "any nonproject insurance" total because some participants obtained both types. | |||
| b. Includes coverage provided by the beneficiary's or spouse's current/former employer, self- or family-paid coverage, and Consolidated Omnibus Budget Reconciliation Act of 1985 (COBRA) plans. | |||
| c. Includes Medicare, Medicaid, Medi-Gap, military health care, Indian Health Service, workers' compensation, and other state programs. | |||
Use of Medical Services
Participants in the project's treatment group took advantage of the available medical services within the first 6 months of enrollment. The use of health care services shown in Table 9 reflects the fact that the participants had health conditions that needed medical attention. Within 6 months of random assignment, 91.9 percent of the treatment group had seen a doctor, and 90.2 percent reported regular use of prescription drug benefits. Emergency room visits were reported by 36.6 percent of treatment group members, and 23.3 percent had been admitted to the hospital.
| Service | AB and AB Plus combined | Control group | P-value |
|---|---|---|---|
| Ambulatory care | |||
| Saw a doctor | 91.9 | 84.9 | 0.020** |
| Had a regular source of care | 82.3 | 71.7 | 0.010*** |
| Number of visits | |||
| 1 or 2 visits | 22.3 | 30.0 | 0.060* |
| 3 or more visits | 60.0 | 41.9 | <0.001*** |
| No regular source of care | 17.8 | 28.0 | 0.010*** |
| Changed source of usual medical care in the past 6 months | 13.3 | 6.4 | 0.020** |
| Saw an internist, general practitioner, or family doctor | 67.1 | 57.0 | 0.020** |
| Saw a specialist or another type of doctor | 67.4 | 61.6 | 0.180 |
| Saw a psychologist, psychiatrist, or social worker | 22.6 | 23.3 | 0.840 |
| Regularly took prescription medications | 90.2 | 80.0 | 0.002*** |
| Nonambulatory care | |||
| Visited emergency room | 36.6 | 27.8 | 0.040** |
| 1 or 2 times | 34.2 | 27.6 | 0.130 |
| 3 or more times | 2.1 | 0.5 | 0.150 |
| Never visited emergency room | 63.7 | 71.9 | 0.060* |
| Admitted to hospital | 23.3 | 15.8 | 0.040** |
| 1 or 2 times | 22.8 | 13.8 | 0.014** |
| 3 or more times | 0.4 | 2.1 | 0.080* |
| Never admitted to hospital | 76.9 | 84.1 | 0.015* |
| Sample size | 289 | 194 | |
| SOURCE: Mathematica Policy Research, Inc., AB demonstration project 6-month followup survey, October 2008–January 2009. | |||
| NOTES: Estimates are regression adjusted to account for chance baseline differences across the study groups and weighted for nonresponse. The p-value column represents the probability that the differences between the characteristics of the treatment and control groups are different from zero. A small percentage of cases had missing values; these were interpreted as nonusage. | |||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance levels are indicated as * = 10 percent, ** = 5 percent, and *** = 1 percent. | |||
Although the reported use of medical services differs between the treatment group and the control group, almost the same share—84.9 percent—of the control group saw a doctor during this period; and while 82.3 percent of the treatment group reported a "regular source of care," 71.7 percent of the control group also responded affirmatively. However, while exactly 60 percent of the treatment group reported three or more visits during this 6-month period, only 41.9 percent of the control group reported that level of care. Thus, although both groups reported they were able to obtain medical care, their responses seem to indicate that health insurance may provide access to a higher level of service, which might result in fewer "unmet needs."
It is frequently reported that uninsured people often use the emergency room for routine health care issues; however, the survey surprisingly showed higher levels of emergency room use in the treatment group (36.6 percent) than in the control group (27.8 percent). The difference in hospital admissions was in the expected direction: Only 15.8 percent of the control group was admitted to a hospital, and 23.3 percent of those with health insurance had been admitted.
Unmet Medical Needs
Participants were asked specific questions about whether they either postponed or went without medical or prescription needs. As Table 10 shows, the frequency of reported unmet medical needs for any reason was substantially lower for the treatment group (45.0 percent) than for the control group (63.8 percent). However, even among those with the AB or AB Plus health plans, a significant percentage reported unmet needs: 51.1 percent reported not filling or refilling a prescription for any reason, 32.2 percent postponed getting medical care, and 19.2 percent did not get medical care. The health plans make a difference, however, as 51.4 percent of the control group did not fill a prescription because of cost, while only 24.8 percent of the treatment group did not fill a prescription because of cost. The difference is smaller for referrals to a doctor for tests or for surgery, and the share of participants in both groups reporting an unmet need is relatively small. In the control group, for example, cost or lack of insurance prevented only 4.0 percent from going to a doctor after being referred, only 7.6 percent did not go for surgery when referred, and only 8.4 percent did not get a test or x-ray after referral.
| Need | AB and AB Plus combined | Control group | P-value |
|---|---|---|---|
| Percentage of participants reporting unmet— | |||
| Medical needs | |||
| Any unmet medical need | 45.0 | 63.8 | <0.001*** |
| Postponed getting medical care | 32.2 | 58.8 | <0.001*** |
| Did not get medical care | 19.2 | 41.5 | <0.001*** |
| Referred to doctor, but did not go | 12.0 | 16.4 | 0.170 |
| Referred for tests and x-rays, but did not go | 4.3 | 9.6 | 0.010** |
| Referred for surgery, but did not go | 13.7 | 10.9 | 0.500 |
| Medical needs due specifically to cost or lack of insurance a | |||
| Did not see or postponed seeing a doctor or receiving medical care | 34.0 | 59.7 | <0.001*** |
| Referred to doctor, but did not go | 3.4 | 4.0 | 0.760 |
| Referred for tests and x-rays, but did not go | 1.4 | 8.4 | <0.001*** |
| Referred for surgery, but did not go | 2.1 | 7.6 | <0.001*** |
| Prescription drug needs b | |||
| Did not fill or refill prescription for any reason | 51.1 | 60.5 | 0.040** |
| Unmet need for prescription drugs because of cost | 24.8 | 51.4 | <0.001*** |
| Did not take prescription for noncost reasons | 40.1 | 32.6 | 0.090* |
| Average monthly out-of-pocket costs for prescriptions exceeded $100 | 12.5 | 31.1 | <0.001*** |
| Sample size | 289 | 194 | |
| SOURCE: Mathematica Policy Research, Inc., AB demonstration project 6-month followup survey, October 2008–January 2009. | |||
| NOTES: Estimates are regression adjusted to account for chance baseline differences across the study groups and weighted for nonresponse. The p-value column represents the probability that the differences between the characteristics of the treatment and control groups are different from zero. A small percentage of cases had missing values; these were interpreted as not having an unmet need. | |||
| A chi-square test for categorical variables and a t-test for continuous variables were run to determine whether there was a difference in the distribution of the characteristics across study groups. Statistical significance levels are indicated as * = 10 percent, ** = 5 percent, and *** = 1 percent. | |||
| a. Unmet needs are attributed to cost if the respondents reported they did not get care because they did not have health insurance, they could not afford the copay, or the provider did not accept insurance. | |||
| b. Includes delaying or not refilling a prescription, or taking less than the prescribed dosage. | |||
In summary, two surprising findings from the 6-month survey are that (1) 24.2 percent of the control group were able to obtain health insurance within 6 months of random assignment, and (2) the control group generally received needed medical care, albeit at a somewhat lower rate, despite not having access to the AB package.
Health Benefit Expenditures
The costs of providing accelerated health benefits were higher than we expected. As the project began, we estimated that the costs of providing the AB package would be about $24,000 per person from the time of enrollment to the end of the 24-month Medicare waiting period. We based our estimate on recent studies that used secondary data sources to estimate the costs of the waiting period.20 Our data show that the actual per-person costs exceed $30,000. About 30 percent of the total costs are due to the 9.0 percent of the treatment group members who reached the $100,000 cap that we placed on the AB package.
We examined the characteristics of those who reached the cap to better understand why they reached the maximum. Five diagnostic categories account for 79.3 percent of those reaching the maximum (Table 11). Nearly 24 percent of the participants reaching the maximum have a malignant neoplastic disease, 18.5 percent have cardiovascular conditions, and 13.0 percent have neurological impairments. The mental disorders and musculoskeletal impairment categories each account for an additional 12.0 percent.
| Primary diagnosis | Number | Percentage distribution | Percentage within the primary diagnosis group |
|---|---|---|---|
| Cardiovascular impairments | 17 | 18.5 | 21.3 |
| Malignant neoplastic diseases | 22 | 23.9 | 22.7 |
| Mental disorders | 11 | 12.0 | 5.0 |
| Musculoskeletal impairments | 11 | 12.0 | 5.6 |
| Neurological impairments | 12 | 13.0 | 8.7 |
| Other | 19 | 20.7 | 6.6 |
| Total | 92 | 100.0 | 9.0 |
| SOURCE: Authors' calculations based on data from the AB demonstration project. | |||
| NOTE: Totals do not necessarily equal the sum of rounded components. | |||
We also examined the incidence of reaching the cap for each diagnostic category identified in Table 11. Of all participants with malignant neoplastic disease (cancer), 22.7 percent reached the cap. Participants with a cardiovascular impairment were a close second, with 21.3 percent reaching the maximum.
The speed with which AB beneficiaries reached the maximum benefit indicates additional costs they would have incurred during the rest of the waiting period. On average, these participants reached the limit in just over 12 months. Because this period may vary by health condition, we calculated the average time for each diagnostic category. Chart 5 shows a box and whiskers plot of these data. On average, participants with malignant neoplastic disease reached the maximum sooner than beneficiaries with other primary diagnoses. The median period for reaching the maximum benefit for participants with malignant neoplastic diseases was just 9 months after random assignment into the project. We conclude that without the $100,000 limit, costs might have been substantially higher given the length of time left in the waiting period.
Number of months to reach the $100,000 spending limit, by primary diagnosis
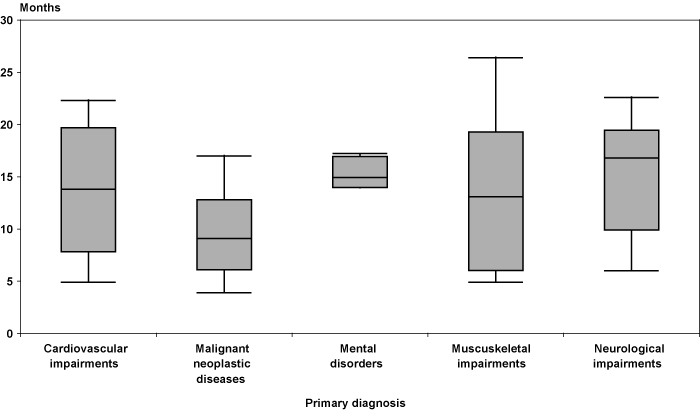
| Cardiovascular impairments | Malignant neoplastic diseases | Mental disorders | Muscuskeletal impairments | Neurological impairments | |
|---|---|---|---|---|---|
| Lower adjacent value | 4.9 | 3.9 | 13.94 | 4.9 | 6.0 |
| 25th percentile | 8.8 | 6.8 | 13.94 | 6.4 | 11.2 |
| Median | 13.8 | 9.1 | 14.92 | 13.1 | 16.8 |
| 75th percentile | 18.8 | 11.4 | 16.83 | 16.9 | 18.4 |
| Upper adjacent value | 22.3 | 17.0 | 17.23 | 26.4 | 22.6 |
One explanation for the substantial share of participants reaching the maximum is the costliness of end-of-life care. The two most prevalent conditions among beneficiaries who reach the maximum, malignant neoplastic disease and cardiovascular conditions, have relatively high short-term mortality rates. About 45 percent of individuals with malignant neoplastic disease and about 9 percent of those with cardiovascular conditions died during the Medicare waiting period, both exceeding the overall incidence of 7.8 percent. We suspect that the cost estimates we used to budget for the AB project did not properly account for end-of-life care expenses. More conclusive analysis will require information on the full medical costs, which will become available at the end of the project.
Discussion and Conclusions
Congress authorized SSA to conduct a demonstration project to assess the relative benefits and costs of altering the 24-month Medicare waiting period for DI beneficiaries. With this authority, SSA designed and conducted the Accelerated Benefits demonstration. Prior to conducting the study, we examined available information on the Medicare waiting period from news stories, qualitative and quantitative research, and the "purpose and findings" section of the Ticket to Work and Work Incentives Improvement Act.21 Based on this information, we expected to find that many beneficiaries would not have health insurance coverage, and would not be able to obtain it, during the waiting period. We expected that the AB package would increase the use of health care services by beneficiaries and reduce their unmet medical needs during the first 6 months of the AB demonstration. We also expected that the majority of beneficiaries who did not have health insurance would have very limited access to health care during the waiting period.
According to the 6-month survey, our contractor and subcontractors delivered the AB services to almost all eligible beneficiaries and the vast majority of beneficiaries were satisfied with them. The data show that within 6 months of AB enrollment, about 87 percent of participants who were eligible for services received them, and over 90 percent of the group receiving services reported satisfaction with them. We are therefore confident that the findings from the AB demonstration are unlikely to be affected by any problems with the administration of services.
Only 12.7 percent of beneficiaries identified for the study did not have health insurance coverage at the time we contacted them, and almost 25 percent of them were able to obtain it by the time we recontacted them 6 months later. We suspect this may stem from our selection of beneficiaries who quickly had a favorable outcome on their initial disability decision; that is, it excluded beneficiaries who did not receive a benefit award until after the 6th month of DI entitlement.22 Individuals with health insurance coverage might have complete medical evidence, making it easier for the disability examiner to decide favorably on their case. If our suspicions are correct, then eliminating the Medicare waiting period may help some beneficiaries but it may not close the gap in their health insurance coverage. The provisions for wider health care access in the recently passed Affordable Care Act might fill the gap more effectively. Indeed, our baseline data on the household income of AB participants indicate that the majority would be eligible for subsidies under the new law.
Our data show that the AB package increased access to medical care and reduced unmet medical needs. Although the effects were substantial in some cases, we expected to see larger differences in these outcomes. Our hypothesis was that, without the AB package, few beneficiaries would report having access to medical care and almost all would report some type of unmet medical need. In fact, we found that some who did not have the AB package were able to obtain health care and had only modest levels of unmet medical needs in the first 6 months of the study. In future research, we hope to examine the ways that beneficiaries without health insurance obtain health care and the resulting economic impact.
The costs of providing accelerated health benefits were higher than we expected. At the onset of the project, we estimated that the costs of providing the AB package would be about $24,000 per person. Our data show that actual costs are over $30,000 per person. About 30 percent of the total costs are due to the 9.0 percent of the sample who reached the $100,000 cap that we placed on the AB package. Most of these expenditures appear to be driven by end-of-life care for those with various types of cancers (neoplasms) or with cardiovascular conditions. Without the $100,000 cap, the costs of providing accelerated health benefits would be substantially higher.
We did not expect to see a substantial change in employment or benefit receipt within the first 6 months of the project, and we did not include questions on preventive care and relative quality of care in the 6-month follow-up survey. We expected that most newly entitled beneficiaries would need time to obtain the health care needed to address their disabling condition, seek rehabilitation services, and adjust to their disabling condition. In future research, we plan to use the 12-month follow-up survey to examine the impact of the AB health plan on preventive care and relative quality of care. We also plan to study the longer-term effect of AB on employment and benefit use. We are particularly interested in potential reductions in post-waiting period Medicare expenditures resulting from the care provided through accelerated health benefits.
This article presents data from the early stages of the project. We will have more project information in 2011 when MDRC completes its final report. However, we will continue to examine the impact of AB on long-term employment and program participation outcomes after the final report is released.
Notes
1 Social Security Act Section 223(d)(1) defines a disability as the inability to engage in any substantial gainful activity either "by reason of any medically determinable physical or mental impairment which can be expected to result in death or which has lasted or can be expected to last for a continuous period of not less than 12 months" or because of blindness. The 24-month Medicare waiting period is waived for beneficiaries with end-stage renal disease or Amyotrophic Lateral Sclerosis, and for some beneficiaries with a prior entitlement due to disability. For more information on the history of the 24-month Medicare waiting period, see Szymendera (2007).
2 COBRA allows individuals to continue health insurance coverage through an employer's group plan for 18 months. Individuals may be required to pay the entire premium (that is, their share and the employer's share) plus a 2 percent administrative fee. The law allows DI beneficiaries to continue coverage for 11 additional months, but the costs can increase to 150 percent of the premium during the 11-month extension. Although the 2009 economic stimulus package included federal subsidies of COBRA covering certain individuals who lost a job, it did not include special provisions for DI beneficiaries.
3 In this article, "we" refers broadly to the SSA Office of Program Development and Research team that oversees the AB demonstration.
4 See Stapleton and others (forthcoming) for more information on the relationship between age and employment among DI beneficiaries.
5 See Riley (2006) for more information on the relationship between health insurance status and unmet medical needs among DI beneficiaries.
6 Members of our technical advisory panel include John F. Burton, Jr., Walton Francis, Larry Fricks, Jay Himmelstein, John D. Kemp, Richard Luecking, Joseph Newhouse, Mary Beth Senkewicz, and Michael Sullivan.
7 Emergency situations were an exception to this rule. POMCO, an AB subcontractor, received many requests for gastrointestinal bypass surgery. POMCO denied these requests and this surgery was eventually excluded.
8 Coaches are social workers and psychologists.
9 For more information on estimating induced entry, see Moffitt (1992) and Tuma (2001).
10 We accepted the beneficiaries' self-reported health insurance status because we had no avenue of independent verification. Beneficiaries who completed the baseline survey received $20 for participating.
11 Because there were 66 Phase 1 beneficiaries, only 1,934 Phase 2 beneficiaries were needed to reach the recruitment goal of 2,000. We ultimately enrolled 1,939 Phase 2 beneficiaries.
12 The drawback of recruiting from major metropolitan areas is that rural areas are underrepresented in the sample. We considered drawing a nationally representative sample, but MDRC advised using a purposeful sample based on (1) the need to identify a sample of 2,000 beneficiaries, (2) service delivery burden, and (3) the costs of follow-up data collection activities. Our final sample provides regional diversity, and the areas covered represent a large share of the beneficiary population.
13 Some beneficiaries do not have a Medicare waiting period (see note 1), and others may meet the eligibility standards to qualify for Medicaid coverage.
14 As a neoplasm is an "abnormal growth or mass of body tissue," this diagnostic category includes malignant cancers.
15 See http://www.healthcare.gov/ for more information about the Affordable Care Act.
16 Most had had coverage through Medicaid and no longer met the income limits for Medicaid eligibility.
17 We used a subsample of the early AB enrollees for this survey because the primary purpose was to assess the administration of AB services.
19 Because the satisfaction rates were mostly over 90 percent, we did not include them in Table 7. The results are available from the authors upon request.
19 Some control group members reported both public and private health insurance coverage.
20 Our original estimate exceeds Riley's (2004) estimate of $10,055 (in 2000 dollars), but his estimate does not include the Medicare Part D benefit. After inflating our estimate to account for rising health care costs and the cost of Medicare Part D, our original estimate was similar to the $18,854 (in 2006 dollars) estimated by Livermore, Stapleton, and Claypool (2009), which also accounts for the Part D benefit.
21 In addition to the sources cited elsewhere in this article, see Williams and others (2004) and Hayes, Beebe, and Kreamer (2007).
22 Individuals who were awarded benefits after appealing the initial decision are not included in our sample.
References
[CCD] Consortium for Citizens with Disabilities. 2008. Statement of principles: Social Security disability program work incentives and related issues. Available at http://www.c-c-d.org/task_forces/social_sec/CCD-Principles-and-Recom-29-08.pdf.
Hayes, Robert M., Deane Beebe, and Heidi Kreamer. 2007. Too sick to work, too soon for Medicare: The human cost of the two-year Medicare waiting period for Americans with disabilities. New York, NY: The Commonwealth Fund. Available at http://www.commonwealthfund.org/Content/Publications/Fund-Reports/2007/Apr/Too-Sick-to-Work--Too-Soon-for-Medicare--The-Human-Cost-of-the-Two-Year-Medicare-Waiting-Period-for.aspx.
Livermore, Gina, David Stapleton, Henry Claypool. 2009. Health insurance and health care access before and after SSDI entry. New York, NY: The Commonwealth Fund. Available at http://www.commonwealthfund.org/Content/Publications/Fund-Reports/2009/May/Health-Insurance-and-Health-Care-Access-Before-and-After.aspx.
Moffitt, Robert. 1992. Evaluation methods for program entry effects. In Evaluating welfare and training programs, eds. Charles F. Manski and Irwin Garfinkel, 231–252. Cambridge, MA: Harvard University Press.
Riley, Gerald F. 2004. The costs of eliminating the 24-month Medicare waiting period for Social Security disabled-worker beneficiaries. Medical Care 42(4): 387–394.
———. 2006. Health insurance and access to care among Social Security Disability Insurance beneficiaries during the Medicare waiting period. Inquiry 43(3): 222–230.
Saker, Anne. 2010. Still waiting: Millions of Americans who qualify for disability must wait two years for Medicare. The Oregonian, June 27. Available at http://www.oregonlive.com/health/index.ssf/2010/06/still_waiting_millions_of_amer.html.
Stapleton, David, Su Liu, Dawn Phelps, and Sarah Prenovitz. Forthcoming. Work activity and use of employment supports under the original Ticket to Work regulations: Longitudinal statistics among new Social Security Disability Insurance beneficiaries. Washington, DC: Mathematica Policy Research, Inc.
Sullivan, Michael J. L., Michael Fuerstein, Robert Gatchel, Steven J. Linton, and Glenn Pransky. 2005. Integrating psychosocial and behavioral interventions to achieve optimal rehabilitation outcomes. Journal of Occupational Rehabilitation 15(4): 475–489.
Szymendera, Scott. 2007. Social Security Disability Insurance (SSDI) and Medicare: The 24-month waiting period for SSDI beneficiaries under age 65. CRS Report for Congress RS22195. Washington, DC: Congressional Research Service.
Tuma, Nancy. 2001. Approaches to evaluating induced entry into a new SSDI program with a $1 reduction in benefits for each $2 in earnings. Unpublished manuscript, Stanford University.
[University Centre] University Centre for Research on Pain and Disability. 2010. The Progressive Goal Attainment Program (PGAP). Available at http://www.pdp-pgap.com/pgap/en/index.html.
Williams, Bob, Adrianne Dulio, Henry Claypool, Michael J. Perry, and Barbara S. Cooper. 2004. Waiting for Medicare: Experiences of uninsured people with disabilities. New York, NY: The Commonwealth Fund. Available at http://www.commonwealthfund.org/Content/Publications/Fund-Reports/2004/Oct/Waiting-for-Medicare--Experiences-of-Uninsured-People-with-Disabilities.aspx.